Quick version
What is Ankylosing Spondylitis?
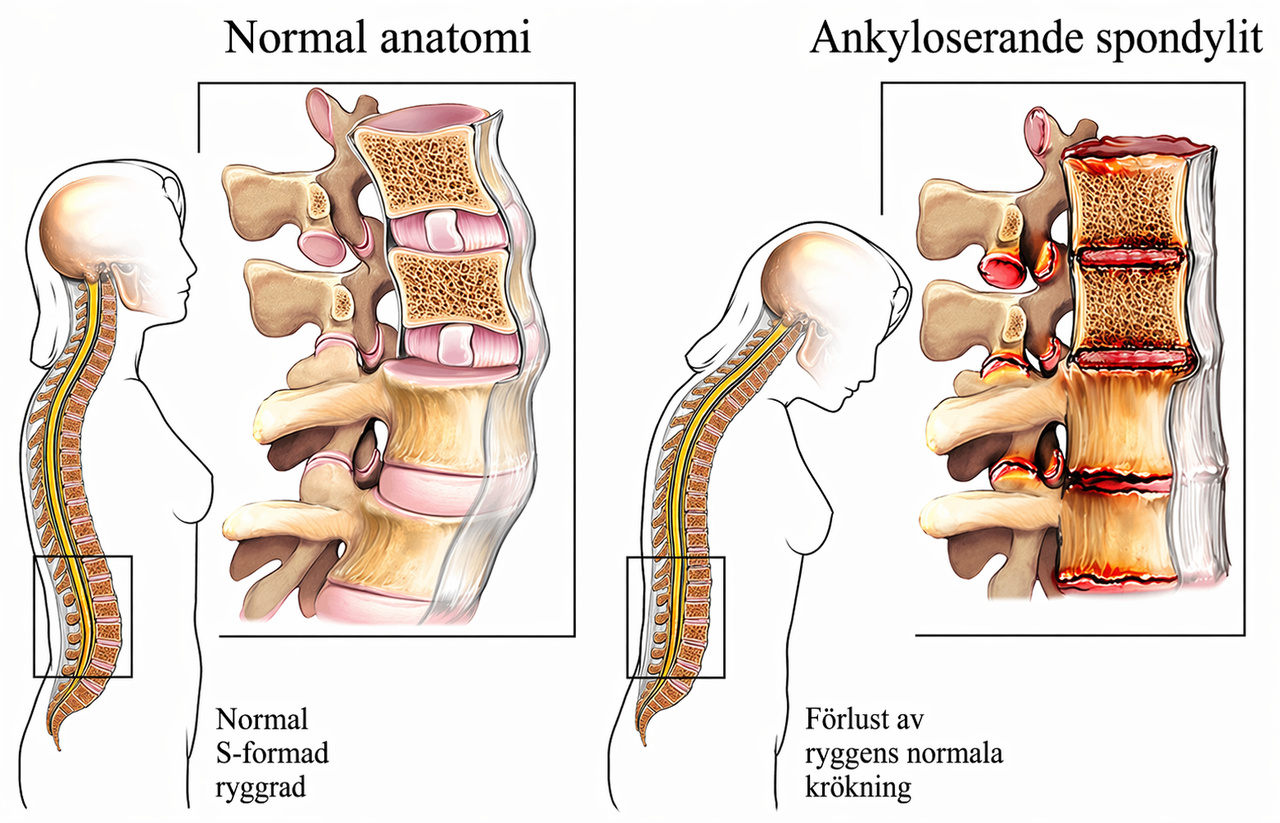
Ankylosing spondylitis is an autoimmune disease where the body's immune system attacks the areas where tendons and ligaments meet bone, especially in the spine and sacroiliac joints. The name comes from the Greek "ankylos" (stiff/fused) and "spondylos" (vertebra). Long-term inflammation can lead to new bone formation, causing vertebrae to fuse and the spine to become rigid. It usually debuts in young adulthood, typically before age 40.
How does Ankylosing Spondylitis feel?
Symptoms often develop gradually and differ from mechanical back pain by improving with activity. Common symptoms include:
- Gradual back pain: Pain in the lower back and buttocks lasting more than three months.
- Morning stiffness: Pronounced stiffness in the morning often lasting over 30 minutes.
- Nocturnal pain: Pain that wakes the person late at night but eases upon getting up and moving.
- Improvement with movement: Unlike a common back strain, AS pain gets better with exercise and worse with rest.
- Other inflammations: Heel pain (enthesitis), inflammation in large joints (knees/shoulders), or eye inflammation (uveitis).
- Fatigue: A general feeling of tiredness caused by ongoing inflammation.
Why do people get Ankylosing Spondylitis?
The exact cause is unknown, but research points to a combination of genetics and environmental factors:
- Genetics (HLA-B27): The strongest risk factor. Most people with AS carry the HLA-B27 gene, though not everyone with the gene develops the disease.
- Immune system: An imbalance causes the immune system to attack the body's own tissues.
- Gut flora: Studies suggest changes in gut bacteria may play a role in triggering inflammation.
- Gender: The disease is slightly more common in men, though it may be underdiagnosed in women due to differing symptoms.
How is Ankylosing Spondylitis diagnosed?
Diagnosis can take time as back pain is very common. The investigation includes:
- Medical history: Looking for inflammatory back pain patterns (onset before 40, improvement with movement).
- Blood tests: Checking ESR and CRP for signs of inflammation and testing for the HLA-B27 gene.
- MRI: The most sensitive tool for detecting early signs of inflammation in the sacroiliac joints.
- X-ray: Can show advanced changes or bone fusion after long-term disease.
- Physical tests: Assessing spinal mobility and chest expansion.