Quick version
Hydrops means that there is an increased amount of fluid in the knee joint and is a sign that the knee is irritated or affected. It can occur from overload, minor injuries such as meniscus injuries, early osteoarthritis or inflammation.
Common symptoms are swelling, stiffness, pain when carrying weight and reduced mobility. Sometimes the swelling occurs quickly after an injury, but it can also develop gradually over time.
An MRI of the knee can confirm the fluid and, above all, help find the cause behind the problems. If the symptoms do not go away or recur, it may be worth examining the knee further to get the correct diagnosis and treatment.
What is hydrops?
Hydrops is an accumulation of synovial fluid in the joint. This fluid is normally present in small amounts and serves to lubricate the joint and reduce friction. When the joint is irritated or damaged, the production of fluid increases, leading to swelling.
In the knee, this can manifest as a clear swelling, a tense feeling or the joint feeling stiff and difficult to move fully.
Why does hydrops occur in the knee?
The knee joint is particularly prone to developing hydrops, partly because it is one of the body's largest joints, but also because of the high mechanical stress it is exposed to in everyday life. Hydrops occurs when the synovial membrane (synovial membrane) reacts to irritation, damage or inflammation by increasing the production of synovial fluid.
This increase in fluid is basically a protective reaction. Synovial fluid helps to reduce friction, improve the supply of nutrients to the cartilage and create a more favorable environment for healing. At the same time, an increased amount of fluid leads to increased intra-articular pressure, which can cause pain, stiffness and reduced mobility.
Hydrops should therefore not be seen as a diagnosis in itself, but as a sign that something is affecting the joint. The reaction can be relatively non-specific and occur in both acute and chronic conditions, as well as in mechanical and inflammatory influences
Common causes of hydrops
The underlying cause varies depending on age, activity level and any previous knee problems. Some of the most common causes include:
- Overload: Repeated mechanical stress, for example during exercise or prolonged standing/walking, can irritate the synovial membrane and cause a reactive increase in fluid without clear structural damage.
- Meniscus injuries: Degenerative or traumatic changes in the meniscus can give rise to local irritation and secondary hydrops. This is one of the most common causes in both younger and middle-aged patients.
- Ligament and cruciate ligament injuries: Acute injuries to, for example, the anterior cruciate ligament can lead to rapid and sometimes pronounced fluid accumulation, sometimes with blood (hemarthrosis).
- Arthrosis: In early or more advanced cartilage changes, low-grade inflammation in the joint is often seen, which can lead to recurrent hydrops.
- Inflammatory conditions: Conditions such as rheumatoid arthritis or reactive arthritis can cause a more pronounced synovitis with increased fluid production.
- Post-traumatic reaction: After a minor injury or irritation, the joint may react with fluid accumulation even if no clear structural damage can be demonstrated.
In clinical practice, it is often the combination of these factors that is behind hydrops. For example, a mild degenerative meniscus injury in combination with strain can cause reactive fluid accumulation, without a single clear injury dominating the picture.
Hydrops in one knee or both?
If the fluid accumulation is only in one knee, it more often indicates a local cause, such as overload or a structural injury. If both knees – or several joints – are affected, it may instead raise suspicion of a more general or inflammatory disease.
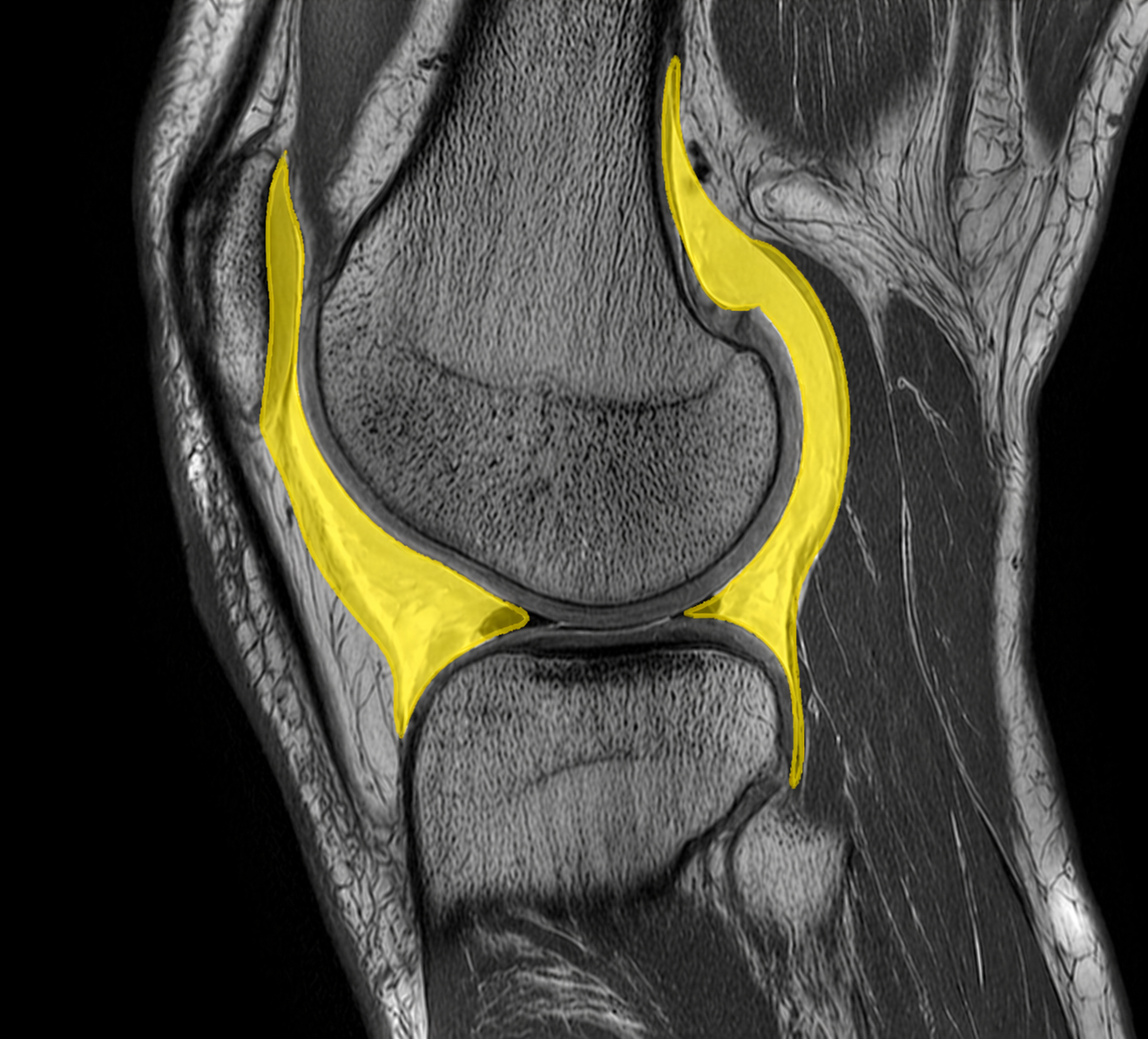
MRI image of the knee joint where synovial fluid (hydrops) is highlighted in yellow. The fluid accumulation is seen intraarticularly and follows the joint capsule around the femoral condyle and tibia, which is typical of inflammation, trauma or other intraarticular irritation.
This difference is important in the medical assessment and affects what further investigation is relevant.
Symptoms of hydrops
Hydrops in the knee often causes a combination of swelling, pain and impaired function. The symptom picture is influenced by both the amount of fluid and the underlying cause. An increased amount of synovial fluid leads to increased intra-articular pressure, which in turn can affect both mobility and the experience of pain.
During clinical examination, you can often see or feel a stretched joint capsule, and in some cases a so-called fluctuation or “ballottement” of the patella can be demonstrated, which indicates a larger amount of fluid in the joint.
- Visible or palpable swelling: The knee may feel enlarged, often with flattened contours around the patella.
- Tension: Increased pressure in the joint gives a feeling that the knee is “full” or tense.
- Stiffness: Especially pronounced after rest, related to both fluid and possible synovitis.
- Pain on exertion: May be due to underlying structural damage or increased pressure in the joint.
- Reduced mobility: Flexion in particular may be limited in larger hydrops.
The onset of symptoms can provide guidance as to the cause. Rapidly occurring swelling, within hours of trauma, for example, indicates a more acute intra-articular injury, such as cruciate ligament injury or hemarthrosis. A more slowly increasing swelling is more common in cases of overload, degenerative changes or low-grade inflammation.
What can an MRI of the knee show in hydrops?
An MRI examination can not only confirm the presence of synovial fluid, but also provide a detailed picture of its distribution and associated changes in the joint. This is crucial for identifying the underlying cause of the hydrops.
On MRI, fluid is seen as a high signal in fluid-sensitive sequences (e.g. T2-weighted images), which makes it possible to distinguish normal amounts from pathological fluid accumulation. At the same time, it is possible to assess whether there are signs of synovitis, capsular involvement or other reactive changes.
Common associated findings in hydrops include:
- Meniscal injuries: Degenerative signal increases or clear ruptures that can cause mechanical irritation and secondary fluid accumulation.
- Ligament and cruciate ligament injuries: Partial or total ruptures, often in combination with increased synovial fluid and sometimes hemarthrosis.
- Cartilage and osteoarthritis changes: Cartilage defects, subchondral involvement and signs of early or established osteoarthritis.
- Synovitis: Thickened and contrast-enhancing synovial membrane in inflammatory conditions.
- Bone marrow edema: May indicate strain-related injury or trauma and is often seen together with hydrops.
MRI thus provides a comprehensive overall assessment of the knee joint and makes it possible to distinguish between a reactive, transient fluid accumulation and an underlying condition that requires targeted treatment or further investigation.
How to interpret the finding of hydrops
Hydrops is in itself a non-specific finding and always needs to be interpreted in relation to symptoms and clinical issues. A small amount of fluid can be a normal reaction after strain, while larger amounts often indicate a more pronounced impact on the joint.
The medical assessment determines whether further investigation is needed or whether the symptoms can be managed conservatively, for example with unloading and physiotherapy.
When should further investigation be carried out?
If the swelling does not go away, recurs or is combined with other symptoms, it may be justified to investigate the knee further.
- Recurrent swelling in the knee
- Long-term pain or stiffness
- Instability or locking
- Swelling after minor exertion
Early evaluation can help identify the cause and reduce the risk of long-term problems.